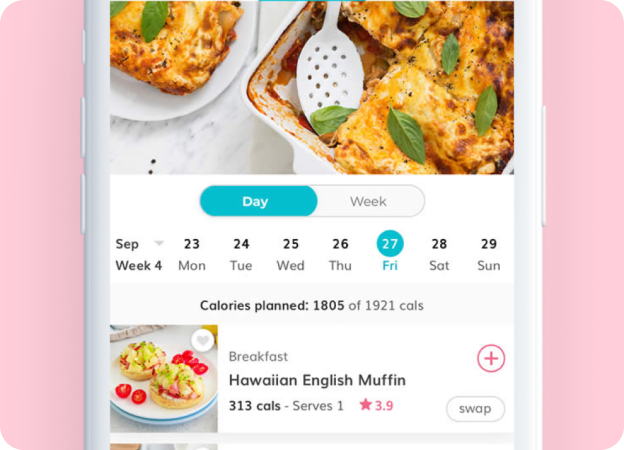
Breastfeeding
Breastfeeding diet plan, tips and advice you will actually use when becoming a new mum. We share with you information on breastfeeding and bottle feeding, remembering there are no rules, only guidelines. Plus great snack ideas you can add to your meal plan whilst you are breastfeeding. The Healthy Mummy online support group for breastfeeding.
7 PAINLESS ways to dry up your breastmilk
For many new mothers, the decision to stop breastfeeding can be an emotional and challenging one. In this blog post, we will guide you through a step-by-step process on how to effectively dry up breast milk.

Pregnant Mum stocks her freezer with heaps of milk boosting snacks ready for baby number 4!
She may be pregnant with baby number FOUR who is due to arrive any day, but that hasn’t stopped Healthy Mummy Cat getting super organised by meal prepping and stocking her freezer with all her favourite Healthy Mummy lactation snacks! And it only took her an hour and a half!

Mothers Day Special: New Mum embarks on Healthy Mummy journey for a second time!
Healthy Mummy Elle has more than one reason to celebrate Mother’s Day this year. With her new baby just 11…

Breastfeeding and weight loss – All you need to know
If you are breastfeeding your baby and do want to lose weight – the good news is that you…

Dark chocolate milk supply boosting muesli bars
Are you a breastfeeding mum looking for a way to give your milk supply a healthy boost? Give these dark chocolate milk supply boosting muesli bars a whirl.

Chocolate Chip Milk Supply Boosting Cookies
If you are you are a breastfeeding mother and you want to eat something healthy and delicious that could also…

Breastfeeding doesn’t always guarantee weight loss. Here’s what you need to know…
One common misconception is that breastfeeding guarantees rapid weight loss. Experts say while nursing does help burn calories, it will make you hungry too.

Mum-of-three loses 20kg AND boosts milk supply by upping her calories
This mum-of-three was hesitant at first to consume the recommended 2,300 calories per day while breastfeeding her second baby.…

What are galactagogues? And how do they affect you?
Midwife, Lactation consultant (IBCLC), Child and Family Health Nurse, baby wearing consultant and mum-of-two, Bel Moore, explains everything you need to…

Can certain foods dry up your breast milk?
Most people know there are a lot of foods with special milk boosting properties but are there any that…

Midwife and lactation expert explains what dream feeding is and how it works
Midwife, Lactation consultant (IBCLC), Child and Family Health Nurse, baby wearing consultant and mum of two, Bel Moore, explains everything mums…

Midwife explains everything you need to know about breastfeeding and weight loss
Weight gain is a normal and necessary occurrence in pregnancy but the reflection of a new postpartum body can shock even the most confident women.

Midwife shares what you need to know about breastfeeding and drinking coffee
Think you have to sacrifice your daily coffee when breastfeeding? Lactation consultant (IBCLC) and midwife Bel Moore gives us…

This mum lost 23kg in 6 months after overcoming breastfeeding issues
Like many mums, Sophie felt exhausted all the time with a newborn. What’s more, she didn’t feel good within…

4 benefits of breastfeeding your baby beyond 12 months
Here at The Healthy Mummy we support healthy breastfeeding, and know that each mum has their own breastfeeding journey. Whether…