Health and Nutrition for Kids
Health and nutrition advice for healthy happy kids. Effective tips for The Healthy Mummy, including handy pointers for the child who won’t sleep and teething babies. Plus diet advice and nutritional information for your baby, toddler, pre-schooler or teen. Your online resource for kids healthy living.

7 ways to boost your immune system when your child joins child care
Does it seem that since your little one has joined daycare they are constantly sick, and in turn, your whole household is too? Here's what to do.

25 Back To School Tricks And Tips
Over the years, this school business gets easier and you learn a few tips and tricks to make life…

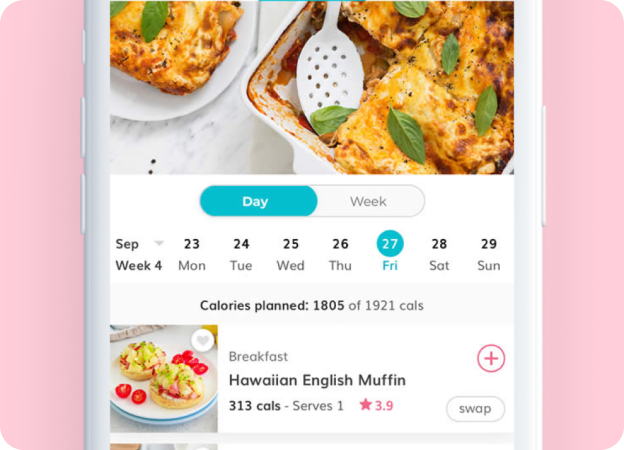
From McDonalds to Subway – we reveal how many calories are in our fave fast foods
Are you one to carefully track your calorie intake no matter where you eat? Find out the calories in some popular Aussie Chains.

Mum shares 10 yummy recipes that her fussy eaters love
Mum Sophie Bellingham shares the ten best recipes from the Healthy Mummy that her fussy eating kids love (and actually eat) that are also good for them.

12 simple lunch box hacks to save you time
We’ve pulled together 12 tried and tested lunch box hacks (from real mums like you) that will give you…
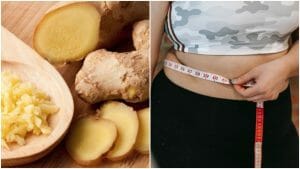
From melting belly fat to reducing bloating and improving digestion -the health benefits of ginger!
Ginger may be the answer to helping banish all your weight loss and bloated belly problems! Get these Healthy Mummy ginger recipes!

Fussy babies tend to turn into intelligent kids, study finds
Do you have a fussy baby? Chances are your little one will end up with a higher IQ than his or her peers, claims a study.

5 HEALTHY and Nut Free Snack Bar Alternatives for the Kids Lunchboxes
Healthy lunchboxes can often be a challenge. To help busy parents, we've gathered five healthy nut-free recipes that are perfect for any lunchbox.

Kids grow taller in the school holidays, claims health expert
Ever wondered why your children seem to outgrow their school uniforms after the summer break and not so much…

URGENT WARNING: Some Easter eggs are choking hazards for young kids
Parents were warned not to purchase hard solid eggs because like grapes, they are a choking hazard.

6 kid-friendly cereals that live up to their low sugar claims
Ever felt a little overwhelmed by all the choices in cereal aisle? Well, here are 6 kid-friendly cereals that live up to their low sugar claims.

Hey Teachers! Food shaming our kids is never the answer
Experts are speaking up about food shaming since schools have banned ham and cheese toasties, fairy bread, juice poppers,…

Why am I always hungry all of the time?
Feeling hungry all the time makes it difficult to concentrate on more important things. Here are the top 10 reasons why you feeling constant hunger.

Financial stress and managing your mental health
Psychologist Dr Bec Jackson offers her practical tips and advice for handling financial stress before it overwhelms your mental health.

The ultimate back to school guide with lunch box recipe ideas, hacks and meal prep tips
With kids heading back to school we thought we would compile the ultimate back-to-school guide to help you survive the chaos. Read t now!